JUMP TO:: MEDICAL + AFFILIATE LINK DISCLOSURES
I’ve been a night owl since second grade.
Not because I was being a bad kid. Not because I was sneaking around. My brain just… never wanted to sleep when it got dark outside. Every summer break I would stay up all night watching TV, get a few hours of sleep, and wake up ready for the day. I was maybe 7 years old. That wasn’t a phase. That was my body telling me something nobody bothered to listen to.
And then school would start back up. 7:20 am bell. Which meant catching the bus before 6 am some mornings. My mom drove me as often as she could because getting me up and functioning that early was a battle neither of us was winning. I was sick constantly. I missed more school than I should have. And not a single person ever connected the dots. Not my parents, not my teachers, not my pediatrician. Nobody looked at this kid who was wide awake at midnight and dragging by 7 am and thought… maybe her body is on a different clock.
It took me until I was an adult, working night shift as a NICU nurse, to finally figure it out.
Night shift was the first time in my entire life that my schedule matched my brain. I had energy. I wasn’t getting sick all the time. While everyone else on the unit was barely functioning, I was thriving. My body finally made sense. And it hit me… my circadian rhythm was never broken. The world just wasn’t built for it.
Why Sleeping on a Night Shift Schedule Still Didn’t Fix My Insomnia
Here’s the thing nobody tells you about being a night owl. Even when your schedule finally matches your body, that doesn’t automatically mean you’re getting quality sleep. It means you’re sleeping at the right TIME. But the quality? That’s a whole different conversation.
I have figured out how to actually fall asleep. Well… sometimes. If I put my phone down and turn on my audiobook, I can usually drift off within a few minutes. But if I won’t put my phone down? No. I’m not falling asleep. My phone is my kryptonite, and I know it.
But falling asleep was never really the main problem. My problem has always been STAYING asleep. Waking up in the middle of the night and then lying there for an hour trying to fall back to sleep after a bathroom break. Watching my brain decide that 3 am is the perfect time to plan tomorrow’s grocery list or replay a conversation from 2009.
And honestly? My sleep history goes darker than that.
After we lost our oldest son, I hit a level of insomnia I didn’t know was possible. I could stay awake for 72 hours straight. Then I’d sleep for maybe 6 hours and do it all over again. I told my doctors. They didn’t do anything. I told them OTC wasn’t working. They shrugged.
Looking back, it was probably depression driving the worst of it. That tracks. It’s never been that severe again. But I have stayed up for over 24 hours more times than I can count… sometimes because my schedule required it, and sometimes because my body just refused to shut down.
Deep Sleep vs. Light Sleep: Why 5 Hours of Quality Rest Beats 8 Hours of Garbage Sleep
Here’s what took me years to understand about my own body.
I function best on 4 to 6 hours of sleep. Always have.
And before anyone comes at me with “you NEED 8 hours”… I have tried. Eight hours makes me feel like I got hit by a truck. I wake up groggy, sluggish, and honestly worse than if I had slept 5. My body does not want 8 hours. It wants 4 to 6 good ones.
I can even function on less for a day or two at a time before I start feeling like I’m coming down with the flu. So my window is already small. Which means every single hour inside that window has to COUNT. There is zero room for garbage sleep. No room for light, surface-level, tossing and turning nonsense where my body never actually gets to the deep stages.
And that need only gets more critical as I get older. Deep sleep naturally declines with age. Perimenopause accelerates that. Stress accelerates it. So I’m working with a short sleep window AND the quality of that sleep is getting harder to protect at the same time. Two forces squeezing from both sides.
This isn’t a story about trying to sleep MORE. This is a story about needing the sleep I get to actually do its job.
And that one sentence is the measuring stick for everything I’ve tried.
Benadryl for Sleep: What Diphenhydramine Actually Does (and the Side Effects Nobody Warns You About)
Most people start with melatonin. I started with Benadryl.
In 2010, my insomnia was at its absolute worst. I hadn’t even heard of melatonin at that point. What I knew was that Benadryl made you drowsy, it was at every pharmacy, and I was desperate. So I started taking it. 25mg at first, and honestly? It usually worked. I could fall asleep.
Benadryl is an antihistamine. It works by crossing into your brain and blocking histamine, which is one of the chemicals that keeps you awake and alert. It’s a blunt force way to sedate you. You’re not sleeping… you’re chemically unconscious. There’s a difference.
But when you’re running on 72 hours of no sleep and your body won’t shut down no matter what you do? Chemically unconscious sounded pretty good to me.
The problem is your body builds tolerance to antihistamines really fast. After a few nights in a row, your brain gets used to it and you need more to get the same effect. 25mg became 50mg. And eventually 50mg wasn’t enough either.
I’ll be honest. I was taking up to 75mg at a time. And yes, I know. I’m a nurse. Do as I say, not as I do. I knew the recommended dose. I took more anyway because I needed to sleep and nothing else was working.
But the real reason I can’t take Benadryl for more than a few days at a time? The dreams.
If I take Benadryl too many nights in a row, I get the most vivid, intense, realistic dreams. And not fun ones. I’m talking full-blown arguments with my husband that feel 100% real. I wake up genuinely mad at him for something he said… that he never actually said. Because it happened in my dream. Not in real life.
I literally have to warn Rich if I’m going to be taking Benadryl for more than 3 days. “Hey babe, just a heads up, if I wake up mad at you for no reason… it’s the Benadryl. You didn’t do anything.” That is not a sustainable sleep solution. Vivid and disturbing dreams are a known side effect of antihistamine sleep aids, and at 75mg I was basically guaranteeing them.
Diphenhydramine has a half-life of about 4 to 8 hours, which means it clears your system relatively quickly compared to some other options. But “relatively quickly” still means you can wake up feeling groggy, especially at higher doses.
The measuring stick: It knocked me out but didn’t give me quality sleep. Built tolerance fast. And the vivid dream side effects made it unsustainable for more than a few days at a time.
Why Melatonin Didn’t Work for Me (and What It Actually Does)
I didn’t try melatonin until nursing school. That’s when I started bouncing between night and day schedules, and every time my schedule flipped I reached for melatonin thinking it would help me adjust.
It got me to sleep. But I still woke up feeling like I hadn’t slept at all.
Melatonin is a hormone. Your brain makes it naturally when it gets dark outside. Its entire job is to signal your body that it’s time to sleep. That’s it. Think of it like a “closed” sign on a store. It tells the world the store is shut down for the night.
But whether the cleaning crew actually shows up to do the overnight work? Melatonin has nothing to do with that.
The “cleaning crew” is deep sleep. Stage 3. Delta wave sleep. That’s where your brain consolidates memories, your immune system does its thing, your hormones get regulated, tissue gets repaired. ALL of that happens in deep sleep. And melatonin doesn’t touch it. At all.
So I was putting up the “closed” sign every night. But the cleaning crew never showed up.
There’s also a timing problem that nobody talks about. Melatonin works by responding to darkness. If you’ve spent 35 years training your brain to ignore the “it’s dark outside” signal… your body is just going to blow right past that melatonin like it’s not even there. It’s not a sedative. It’s a suggestion. And my body has been ignoring that suggestion since I was 7.
A meta-analysis of 19 randomized controlled trials found that melatonin supplements helped people fall asleep about 7 minutes faster and sleep about 8 minutes longer than a placebo. Seven minutes. That’s it. For most people dealing with real sleep issues, that’s barely a dent.
And here’s the part that really gets me as a nurse. Melatonin is not regulated by the FDA. It’s sold as a supplement, not a medication. A 2023 study published in JAMA looked at 25 melatonin gummy products and found that 22 of them contained different amounts of melatonin than what the label said. Some had nearly 3.5 times the labeled amount. You don’t actually know what you’re taking.
The measuring stick: Did melatonin help me get quality, restorative sleep in my 4 to 6 hour window? No. It suggested sleep. It never delivered depth.
Olly Sleep Gummies Review: Still Just Melatonin in a Prettier Package
After plain melatonin didn’t cut it, I tried the Olly Sleep gummies. The ones with melatonin plus L-theanine, chamomile, passionflower, lemon balm… all the “calming” botanicals.
I’ll give them this: they’re tasty. And I figured they weren’t hurting anything. So I kept taking them alongside whatever else I was using at the time. But the quality of sleep? Still garbage. I was still waking up feeling like my body never actually got to the deep stages.
It’s still melatonin-based. The add-in ingredients may help with relaxation, and some of them have mild evidence for calming the nervous system. But none of them are changing your sleep architecture. None of them are getting you into deeper sleep stages. It’s the same traffic cop in a fancier uniform.
The measuring stick: Slightly better packaging, same result. My body still wasn’t getting the deep, restorative sleep it needed.
Unisom vs. Benadryl for Sleep: Doxylamine Succinate vs. Diphenhydramine
By this point I was combining melatonin (or the Olly version) with 75mg of Benadryl. Yes, again with the 75mg. I know. Nurse brain knows better. Desperate-for-sleep brain does not care.
When even that combo wasn’t cutting it anymore, I swapped the Benadryl out for Unisom SleepTabs. Doxylamine succinate. Same family of antihistamines, but this one is the heavy hitter. I still took the melatonin alongside it, though honestly I couldn’t tell a difference with or without it at that point.
The biggest difference between Unisom SleepTabs and Benadryl is the half-life. Doxylamine hangs around in your system for 10 to 12 hours. It will absolutely knock you out cold. But when that alarm goes off the next morning? You feel like you’re walking through concrete. The next-day hangover from doxylamine is brutal.
Everything else is the same problem. It’s still blocking histamine to force sedation. It’s still not improving sleep quality or depth. Your body still builds tolerance. You’re still chemically unconscious, not restored.
And for anyone working 12-hour shifts where you have to be sharp and alert and making critical decisions? That next-day fog is dangerous. I cannot afford to be operating in a haze when I’m taking care of sick and premature infants. Period.
The measuring stick: Stronger sedation, longer hangover, same lack of actual deep sleep. Not the answer.
Why OTC Sleep Aids Never Fixed My Sleep Quality
Here’s what I wish somebody had explained to me years ago, instead of letting me fumble through the pharmacy aisle trying to figure it out on my own.
Everything I tried was doing one of two things. Either it was SUGGESTING sleep (melatonin and its fancier versions) or it was FORCING sedation (antihistamines like Benadryl and Unisom).
Neither one was addressing the actual quality of my sleep. Neither one was helping my body get into deep, restorative delta wave sleep. They were either putting up the “closed” sign or knocking me unconscious. But the cleaning crew… the part where my body actually does the repair work, consolidates memories, regulates hormones, restores itself… that part never showed up.
I spent years cycling through the same two categories of sleep aids and wondering why I still felt exhausted. The answer was that I was solving the wrong problem the entire time.
I didn’t need help falling asleep. I needed help sleeping DEEPLY.
Sermorelin for Sleep: The Peptide That Actually Helped Me Stay Asleep
I didn’t start Sermorelin for sleep.
I started it for completely different reasons. But one of the first things I noticed? I was falling asleep easier. And when I woke up in the middle of the night for a bathroom break, I could actually fall back to sleep instead of lying there staring at the ceiling for an hour while my brain ran tomorrow’s to-do list.
That was huge for me. Falling back to sleep after waking up had been one of my biggest struggles for years. And Sermorelin quietly fixed it without that even being the goal.
Sermorelin is a growth hormone-releasing hormone (GHRH) analog. It supports your body’s natural production of growth hormone, which plays a big role in recovery, tissue repair, and body composition. Growth hormone release is closely tied to your sleep cycles… your body produces most of it during deep sleep. So it makes sense that supporting GH production would also support the sleep that triggers it.
Unlike everything I tried from the pharmacy aisle, Sermorelin requires a prescription and physician oversight. I get mine through EllieMD, where a licensed provider evaluates you and personalizes your dosing. That’s a completely different experience from grabbing a bottle off a shelf and hoping for the best. And honestly? That’s part of why it actually works. Someone is paying attention to what YOUR body needs, rather than handing you a one-size-fits-all dose.
Sleep isn’t why I started Sermorelin. But sleep is absolutely why I continue to take it. The muscle and body composition benefits are the icing on the cake at this point.
If your main struggle is falling asleep, staying asleep, or falling back to sleep after waking up… Sermorelin might be worth exploring on its own. It made the biggest difference of anything I’ve tried for those specific problems. But if your struggle is more about the QUALITY and depth of your sleep once you’re actually out? Keep reading. Because that’s where my story goes next.
Even with Sermorelin helping me fall asleep and stay asleep better than anything else I’ve tried… my watch data still tells me I’m not consistently getting a lot of deep sleep. The falling asleep part improved. The staying asleep part improved. But the DEPTH? That gap is still there.
Sermorelin got me further than anything in the pharmacy aisle ever did. It was the first time I felt like something was actually working WITH my body instead of just sedating it or suggesting it do something it didn’t want to do. But it wasn’t the complete answer.
The measuring stick: Best results so far. Genuinely helps me fall asleep and fall back to sleep. But my watch data says the deep sleep depth still isn’t where it needs to be. Close… but not all the way there.
What Is Deep Sleep? A Nurse Explains Sleep Stages and Why They Matter
Okay, so I keep saying “deep sleep” like it’s this one magic thing. Let me break down what’s actually happening in your brain when you sleep, because this is the part that changed everything for me.
Your sleep has stages. You cycle through them multiple times every night.
Stages 1 and 2 are light sleep. Your body is transitioning, slowing down, but you’re not doing the heavy repair work yet. You can be woken up pretty easily. This is where most people spend the majority of their night if their sleep quality is poor.
Stage 3 is deep sleep. Delta wave sleep. This is where the real work happens. Your brain waves slow way down into these big, heavy delta waves. Your brain is consolidating memories. Your immune system is doing its thing. Your hormones are getting regulated. Tissue is getting repaired. Your body is literally rebuilding itself. This is the stage that matters most for waking up feeling like you actually slept.
Then there’s REM sleep, which is where dreaming happens, and your brain processes emotions and experiences.
The first cycle through all of these stages takes about 90 minutes. Then you cycle through again, about 100 to 120 minutes per cycle, after that. In a healthy night of sleep, you’re getting multiple rounds of deep sleep woven into those cycles.
Here’s the problem. Deep sleep is the FIRST stage to get wrecked by stress, hormonal shifts, and age. Perimenopause? Your sleep architecture starts changing before you even realize what’s happening. Chronic stress? Cortisol stays elevated when it’s supposed to drop, and deep sleep suffers. Shift work? Your circadian rhythm is so confused that your body can’t settle into the normal cycling pattern.
You can sleep 8 hours and barely touch Stage 3. You were in the pool all night, but you never went below the surface.
And here’s the other part nobody talks about. Your stress system and your sleep system are supposed to take TURNS. Stress runs the day. Then it clocks out so sleep can take over at night. When that handoff breaks down, you get that “tired but wired” feeling. Exhausted, but your brain won’t stop running the list. That’s not a personality trait. That’s not anxiety being dramatic. That’s a broken shift change inside your body.
This is why the hours don’t matter as much as people think. This is why I feel great on 5 hours and terrible on 8. If my body is efficient at getting into deep sleep during a shorter window, those 5 hours are doing more for me than 8 hours of light, surface-level sleep ever could. But if something is preventing me from reaching that deep stage consistently… it doesn’t matter how many hours I’m in bed. My body isn’t getting what it needs.
And that’s exactly what my watch has been showing me. Even with Sermorelin helping me fall asleep and stay asleep… the deep sleep numbers aren’t always there.
Which brings me to DSIP.
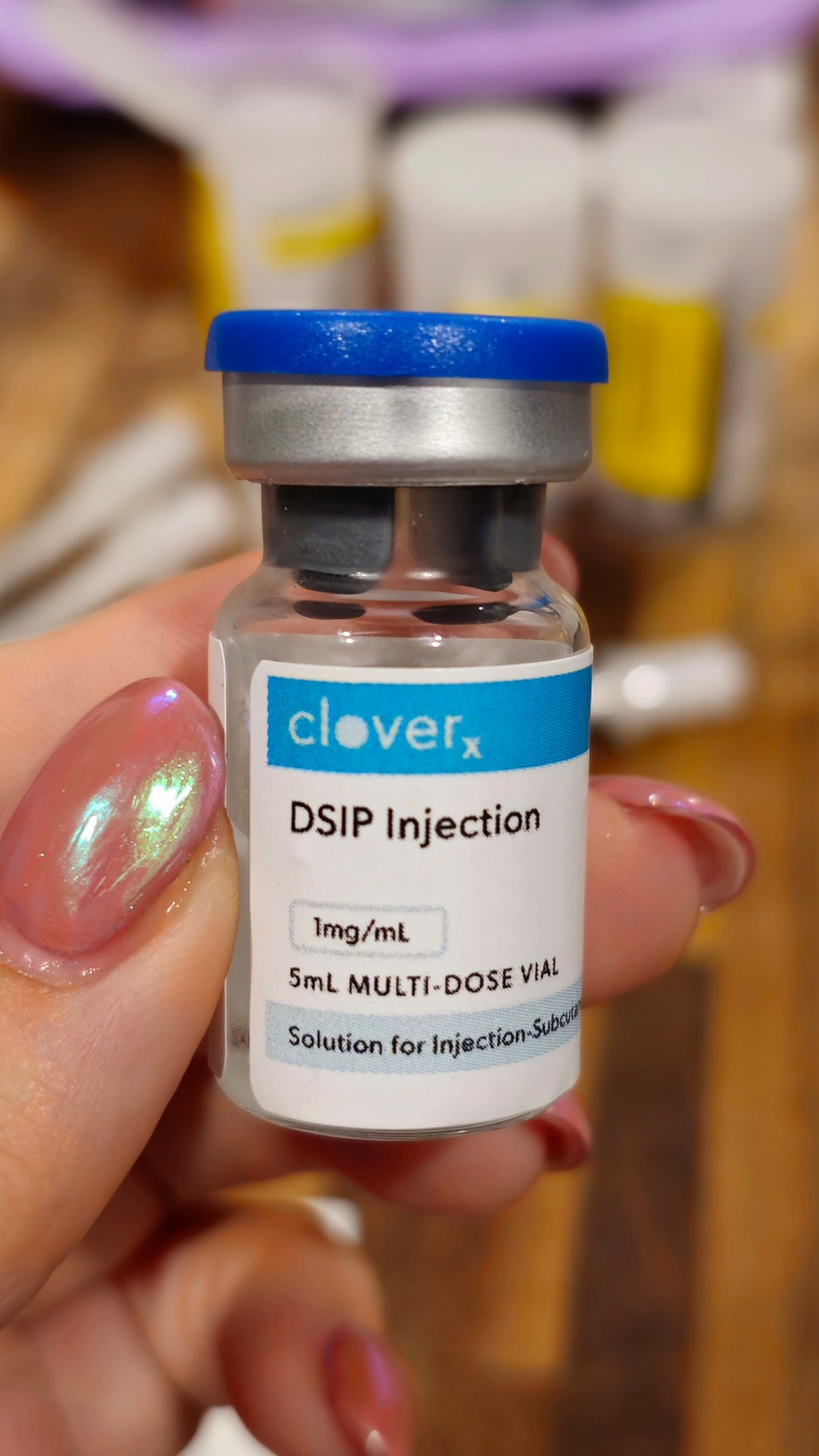
What Is DSIP? The Sleep Peptide Being Studied for Deep, Restorative Sleep
DSIP stands for Delta Sleep-Inducing Peptide. It is literally named after the thing I’ve been chasing this entire time.
It’s a naturally occurring neuropeptide… meaning your body already makes it. It was first discovered in the 1970s when researchers noticed it helped promote delta wave activity in the brain. That’s deep sleep. Stage 3. The cleaning crew. It’s been studied for over 40 years, and the research has looked at its role in sleep regulation, circadian rhythm signaling, stress hormone balance, and neurological resilience.
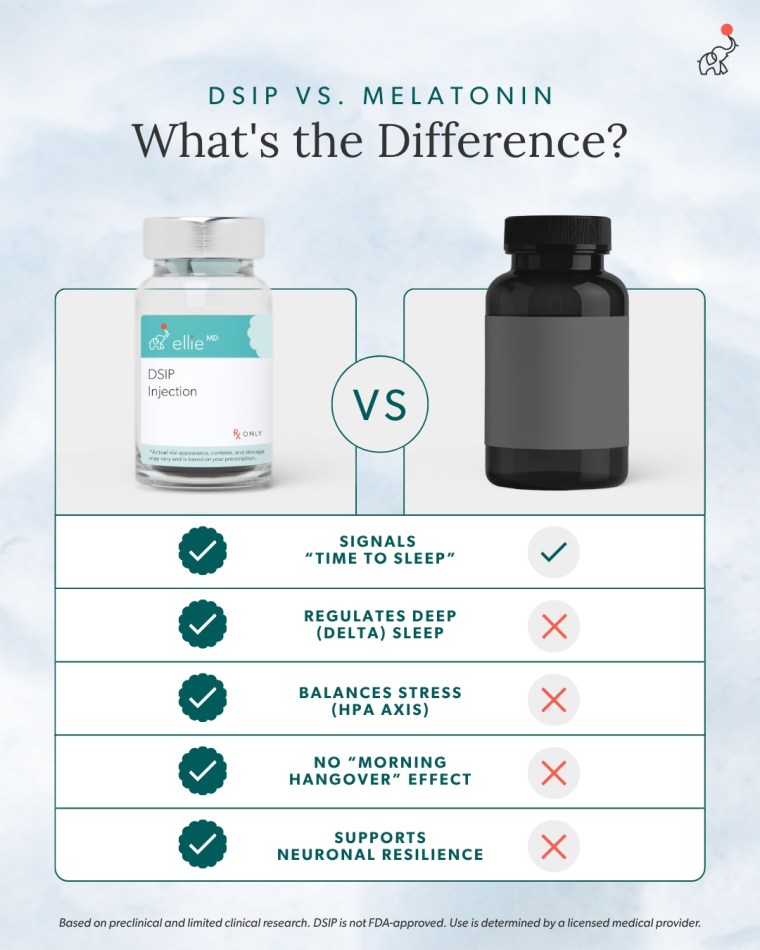
Let me say that again. It’s being studied for sleep DEPTH, circadian rhythm, AND the stress-cortisol connection. All three of the things that have been working against me my entire life.
DSIP is not a sedative. It’s not knocking you out like Benadryl or Unisom. It’s not just suggesting sleep like melatonin. It’s being looked at for helping your brain actually access and maintain those deep, restorative delta wave sleep stages. It may help support the quality of your sleep, not just the timing or the duration.
Remember the stress-sleep handoff I talked about? Where your stress system is supposed to clock out so your sleep system can take over? Research suggests DSIP may help support that handoff by helping regulate cortisol pathways through the HPA axis. So instead of lying there “tired but wired” with your brain refusing to shut down… DSIP may help your body actually make that transition.
And unlike melatonin, which only responds to darkness and has nothing to do with what happens after you fall asleep… DSIP is being studied for what happens DURING sleep. The architecture. The depth. The repair work. The part that actually matters for how you feel when you wake up.
Here’s what the research shows so far. A double-blind study on chronic insomnia patients found improved sleep efficiency and shorter time to fall asleep with DSIP compared to placebo. Animal studies have shown DSIP’s ability to increase delta wave sleep without suppressing REM, meaning it may help enhance sleep quality rather than just sedating the subject. Research has also shown it may help support the body’s response to stress, with studies noting what researchers described as decreased stress markers and improved stress tolerance.
Is the research perfect? No. The human trials are small and some of the data is older. There are scientists who think DSIP is the real deal and scientists who think the evidence is inconclusive. I’m being straight with you about that because I’m always going to keep it real. But for someone like me… a lifelong night owl with a short sleep window who needs every hour to count, who has tried everything in the pharmacy aisle and hit a wall, who is already seeing real benefits from Sermorelin but still has a gap in deep sleep… the research on DSIP lines up with exactly what I need.
DSIP for Shift Workers and Night Owls: Why I Started It Before Day Shift
When EllieMD added DSIP to their offerings, I was completely stoked. And the timing could not have been better.
I was about to be forced onto day shift for three months. My lifelong night owl brain was about to be shoved onto a schedule that goes against everything my body has ever wanted. I already knew from experience that my sleep quality is historically garbage when I’m on a day shift schedule. Even with Sermorelin helping me fall asleep and stay asleep, forcing my body to sleep during hours it doesn’t want to sleep means those hours are usually light, surface-level, not restorative.
DSIP is being studied for exactly the gap that’s left. If Sermorelin handles the falling asleep and staying asleep part… DSIP may help with the depth and quality of the sleep I’m actually getting. And for someone who runs on 4 to 6 hours, that depth is everything.
But it’s not just about surviving day shift. When I go back to nights, I want to maintain a quality, restorative sleep pattern there too. This isn’t a short-term fix for a temporary schedule change. This is about finally addressing the one part of my sleep that nothing else has been able to touch.
I ordered it. It’s here. And at the time I’m writing this, I’ve taken my first dose. It’s way too early to tell you how it’s working… I’m not going to do that. Y’all know me. I’ll never talk about results I don’t have. But I’m documenting everything, and once I have real experience to share, I’ll write a full blog post about it.
In the meantime, follow me on Instagram @nicoleinscrubs for the most up-to-date stories on how it’s going. That’s where I’ll be sharing the real-time journey as it happens.
Where to Get DSIP With Real Physician Oversight (Not Research Chemical Websites)
This is important and I want to be clear about it.
DSIP is not something you grab off a shelf at the drugstore. It’s not an unregulated supplement where you don’t know what’s actually in the bottle. It requires a prescription from a licensed healthcare provider who evaluates YOUR health history, YOUR needs, and personalizes YOUR dosing.
I get mine through EllieMD, the same provider I use for my Sermorelin and my GLP-1. Every plan is supervised by a licensed physician. The peptides are compounded to pharmaceutical-grade standards, not research grade. They’re tested for potency and purity and triple-purified for safety. The vials arrive ready to use… no home mixing, no guessing.
And here’s the part that honestly sets it apart for me. You get unlimited messaging with your doctor. You can ask a million questions. That’s what they’re there for, and it’s included in the cost of your meds. You’re not paying extra to talk to someone. You’re not waiting 6 weeks for a follow-up appointment to ask one question. You have a provider in your corner who you can actually reach.
There are people all over the internet buying peptides from random research chemical websites with zero physician oversight and calling it biohacking. As a nurse, that makes me genuinely nervous. You don’t know what you’re getting, you don’t know the purity, you don’t have anyone monitoring how your body is responding. Having a real provider in your corner isn’t just safer… it’s the whole point.
Sermorelin, DSIP, or Both? How to Know Which Sleep Peptide Is Right for You
If any of this resonated with you… if you’re the woman sleeping 7 hours and still waking up exhausted, or the night owl who’s been told to “just go to bed earlier,” or the person who’s tried every melatonin and Unisom on the shelf and nothing has actually fixed the quality of your sleep…
Here’s where I’d start.
If your main struggle is falling asleep, staying asleep, or getting back to sleep after waking up… ask about Sermorelin. That’s where I saw the first real change.
If your main struggle is the DEPTH and quality of your sleep… if you’re sleeping enough hours but never actually feeling rested… DSIP may be worth exploring.
If you’re like me, and it’s both? The combination is what I’m testing now, and I’ll be documenting everything.
You can explore it all through my link at elliemd.com/NicoleInScrubs. A licensed provider will evaluate whether any of this is right for YOUR body. Not mine. Not your friend’s. Yours.
And if you’re not sure where to start, take my free quiz and let’s figure it out together.
I’ve spent over 15 years trying to fix my sleep. I tried the melatonin. The gummies. The Benadryl at doses I shouldn’t have been taking. The Unisom that left me in a fog. I found Sermorelin and it changed the game for falling asleep and staying asleep. And now I’m adding DSIP to address the one thing nothing else has been able to touch… the depth.
I’ve taken my first dose. I’ll be back with a full post once I have real results to share. In the meantime, follow along on Instagram @nicoleinscrubs for the real-time updates.
This post contains affiliate links and/or brand partnership content. I may earn a commission at no extra cost to you.
LET’S BE CLEAR ABOUT WHO I AM (AND WHO I’M NOT).
I’m a registered nurse and health coach who shares real, BS-free information about metabolic health, PCOS, perimenopause, and weight loss, because y’all deserve better than vague wellness fluff. But here’s what I need you to know: I am not YOUR nurse. Everything I share here is for educational purposes only. It is not medical advice, it’s not a diagnosis, and it doesn’t create a provider-patient relationship between us. Nothing on this site replaces the care of a licensed provider who actually knows your full health history. The opinions and content here are my own and do not reflect the views of my employer or the hospital where I work.
SCOPE OF PRACTICE.
As a nurse health coach, I can recommend over-the-counter products and supplements that may support your wellness goals. I don’t prescribe specific prescription medications. When it comes to GLP-1s and peptides, what I can do is talk about the science, what’s available, and what may be beneficial, so you can have an informed conversation with your licensed medical provider. The decision about what’s right for your body always belongs to you and your provider. Always consult your licensed provider before starting any prescription treatment — this is not something that should be DIY’d. These statements have not been evaluated by the FDA. Products discussed on this site are not intended to diagnose, treat, cure, or prevent any disease.
TRANSPARENCY.
I only recommend things I actually trust. Most are products I personally use, some are from partners whose clinical standards I believe in. I will always let you know when it’s something I haven’t tried personally. Some links on this site are affiliate links or part of brand partnerships, which means I may earn a commission at no extra cost to you. As an Amazon Associate I earn from qualifying purchases.
RESULTS + TESTIMONIALS.
Any testimonials or results shared on this site reflect individual experiences only. Results are not guaranteed and will vary based on individual circumstances.